THE IMPACT
Resuscitation at birth is common
10 million infants, or 6 to 8% of births, require resuscitation annually around the world. Over 800,000 deaths result from intrapartum-related events (i.e. birth asphyxia) and over 1 million intrapartum stillbirths occur each year. It’s estimated that 30% of these deaths could be saved with higher quality and more broad coverage of neonatal resuscitation training.1
Ventilation forms the cornerstone of resuscitation
The cornerstone of neonatal resuscitation is establishment of effective breathing through manual ventilation. Tidal volumes are not routinely measured during this process meaning there is potential to over-deliver or under-deliver volumes to the infant. Either can lead to serious injury or death.
The current gold standard of care can be improved
In preterm newborns as little as 6 excessive tidal volumes delivered by the resuscitator can initiate severe, even life-threatening lung injury.2 Excessive volumes can lead to pneumothorax or acute respiratory distress syndrome. Significant unrecognised mask leak has also been documented even amongst experienced clinicians.4 Insufficient volumes due to significant mask leak or undetected device failure can also lead to severe morbidity or death.
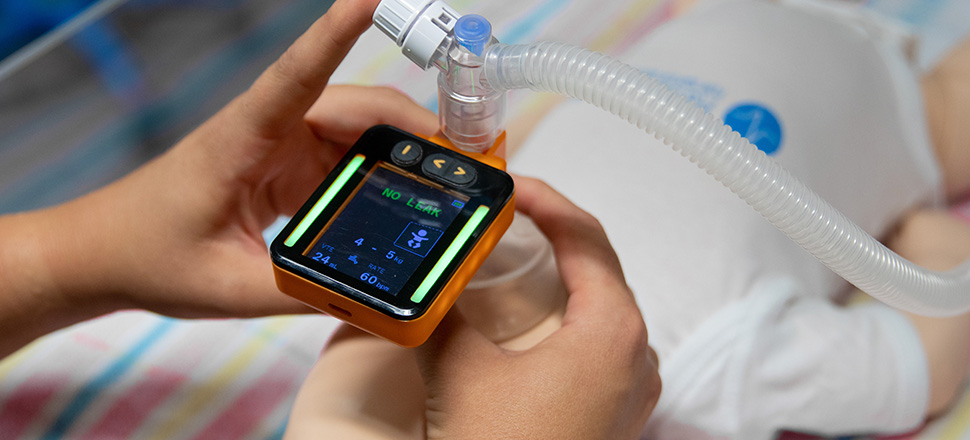
A monitor can help
Training: When clinicians have access to a respiratory function monitor and are aware of the magnitude of mask leak during their training, they are more likely to deliver effective ventilation at the end of the training session.6 The Juno monitor enables more frequent resuscitation practise in line with Australian Resuscitation Council 2016 Guidelines.7
Clinically: A monitor can improve the effectiveness of positive pressure ventilation by providing immediate feedback to the operator.8 The use of a respiratory function monitor reduced leakage from 26.6% to 11.2% in experienced resuscitators.9
Sources
- Lee, A. C., Cousens, S., Wall, S. N., Niermeyer, S., Darmstadt, G. L., Carlo, W. A., … & Lawn, J. E. (2011). Neonatal resuscitation and immediate newborn assessment and stimulation for the prevention of neonatal deaths: a systematic review, meta-analysis and Delphi estimation of mortality effect. BMC public health, 11(3), 1-19.
- Björklund, L. J., Ingimarsson, J., Curstedt, T., John, J., Robertson, B., Werner, O., & Vilstrup, C. T. (1997). Manual ventilation with a few large breaths at birth compromises the therapeutic effect of subsequent surfactant replacement in immature lambs. Pediatric research, 42(3), 348-355.
- Poulton, D. A., Schmölzer, G. M., Morley, C. J., & Davis, P. G. (2011). Assessment of chest rise during mask ventilation of preterm infants in the delivery room. Resuscitation, 82(2), 175-179.
- Wood, F. E., Morley, C. J., Dawson, J. A., Kamlin, C. O. F., Owen, L. S., Donath, S., & Davis, P. G. (2008). Assessing the effectiveness of two round neonatal resuscitation masks: study 1. Archives of Disease in Childhood-Fetal and Neonatal Edition, 93(3), F235-F237.
- Tracy, M. B., Halliday, R., Tracy, S. K., & Hinder, M. K. (2019). Newborn self-inflating manual resuscitators: precision robotic testing of safety and reliability. Archives of Disease in Childhood-Fetal and Neonatal Edition, 104(4), F403-F408.
- O’Currain, E., Thio, M., Dawson, J. A., Donath, S. M., & Davis, P. G. (2019). Respiratory monitors to teach newborn facemask ventilation: a randomised trial. Archives of Disease in Childhood-Fetal and Neonatal Edition, 104(6), F582-F586.
- Australian Resuscitation Council. Australian and New Zealand Committee on Resuscitation Neonatal Guidelines. Melbourne: The Council, 2021. Available from: http://www.resus.org.au/
- Schmölzer, G. M., Kamlin, O. C., Dawson, J. A., Te Pas, A. B., Morley, C. J., & Davis, P. G. (2010). Respiratory monitoring of neonatal resuscitation. Archives of Disease in Childhood-Fetal and Neonatal Edition, 95(4), F295-F303.
- Wood, F. E., Morley, C. J., Dawson, J. A., & Davis, P. G. (2008). A respiratory function monitor improves mask ventilation. Archives of Disease in Childhood-Fetal and Neonatal Edition, 93(5), F380-F381.

